Sudden vision loss is one of the most alarming medical events a person can experience. Whether it affects one eye or both, partial or complete, any abrupt change in vision demands immediate attention.
This guide covers everything you need to know, from causes and warning signs to emergency treatments and prevention. So, you can act fast when every second counts.
Understanding Sudden Vision Loss
Before responding to sudden vision loss, it helps to understand what it actually means and how it presents.
Not all vision loss looks the same, and knowing the difference can help you communicate more effectively with a doctor.
What Sudden Vision Loss Means
Sudden vision loss refers to a rapid decrease or complete absence of vision in one or both eyes, occurring within seconds, minutes, or hours. It is not the gradual blurring that comes with aging or uncorrected prescriptions.
Key distinctions:
- Monocular: Affects only one eye, often points to a retinal or vascular issue
- Binocular: Affects both eyes, may suggest a neurological or brain-related cause
- Transient: Temporary loss lasting seconds to minutes, a serious warning sign
- Permanent: Ongoing loss that does not resolve without treatment
Common Symptoms Patients Notice First
Patients often describe sudden vision loss in different ways. Here are the most commonly reported first signs:
- A dark curtain or shadow falling over part of the visual field
- Sudden blurring or complete blackout in one eye
- Flashes of light followed by a floater storm
- Loss of central vision with intact peripheral vision (or vice versa)
- Double vision appearing without warning
- Graying out of vision during physical exertion
Experiencing sudden blur? Read Why Are My Eyes Blurry Causes Symptoms and When to See an Eye Specialist to know when it is serious.
Major Causes of Sudden Vision Loss
Sudden vision loss is a symptom, not a disease. Several serious underlying conditions can trigger it. Identifying the cause quickly is critical for treatment success.
Retinal Detachment
Retinal detachment occurs when the retina separates from the layer of blood vessels that supplies it with oxygen and nutrients.
It is a true ocular emergency. When the retina detaches, photoreceptor cells start dying within hours, and untreated cases result in permanent blindness.
- More common in highly myopic (nearsighted) individuals
- Often preceded by floaters and flashes of light
- Painless in most cases
Retinal Artery Occlusion (Eye Stroke)
A blockage in the central or branch retinal artery cuts off blood supply to the retina, essentially a stroke of the eye.
It causes sudden, painless, and often complete loss of vision in the affected eye. Time to treatment is critical: the window for intervention can be as short as 90 minutes.
Retinal Vein Occlusion
When a vein draining blood from the retina becomes blocked, blood and fluid leak into the retinal tissue, causing rapid vision distortion or loss.
It is more common in patients with high blood pressure, diabetes, or glaucoma.
Acute Angle-Closure Glaucoma
This form of glaucoma involves a sudden spike in intraocular pressure (IOP). Unlike open-angle glaucoma, it presents dramatically and requires immediate emergency treatment.
If left untreated for even a few hours, it can cause permanent optic nerve damage.
- Symptoms: severe eye pain, headache, nausea, halos around lights
- Vision becomes blurred or foggy rapidly
- The eye appears red and feels hard to the touch
Vitreous Hemorrhage
Bleeding into the vitreous, the gel-like fluid inside the eye, can block light from reaching the retina, causing sudden blurry or hazy vision.
It often appears as a sudden shower of dark spots or floaters. Common causes include diabetic retinopathy, trauma, or a retinal tear.
Optic Neuritis
Optic neuritis is inflammation of the optic nerve, frequently associated with multiple sclerosis (MS) or autoimmune conditions.
It typically affects one eye and may cause pain with eye movement, along with vision loss that develops over hours to days.
Sudden Vision Loss With Pain vs Without Pain
One of the most clinically important distinctions in sudden vision loss is whether it comes with pain. This single factor can dramatically narrow down the possible diagnosis.
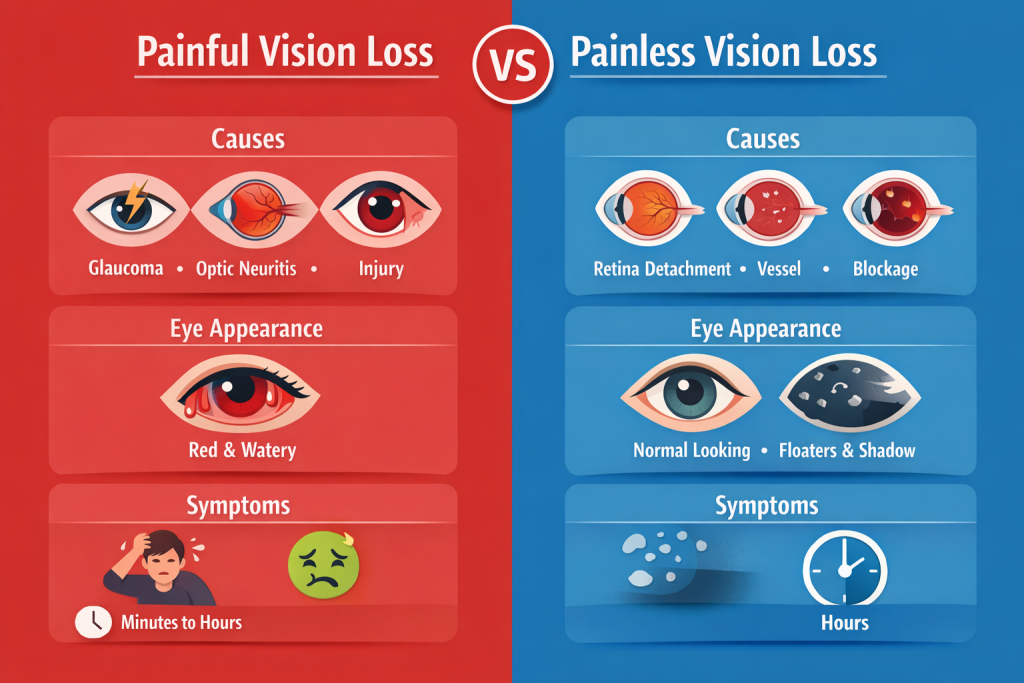
Painful Sudden Vision Loss
Pain alongside vision loss is an urgent red flag. Acute angle-closure glaucoma, for example, is often mistaken for a migraine or stomach upset due to accompanying nausea and headache.
Corneal damage, uveitis, and eye trauma are other painful causes that need same-day emergency evaluation.
Painless Sudden Vision Loss
Painless loss is equally dangerous, and often more deceptive, as patients may delay seeking care. Retinal artery occlusion and retinal detachment are prime examples.
Do not let the absence of pain reassure you. Painless sudden vision loss is always a medical emergency until proven otherwise.
Warning Signs That Need Immediate Emergency Care
Certain symptoms associated with sudden vision loss are absolute indicators that you need to go to the emergency room or call an ophthalmologist right away. Never wait to see if these resolve on their own.
Flashes, Floaters, and Curtain-Like Shadows
These three symptoms together, especially when new and sudden, are classic warning signs of retinal detachment or tear.
- Flashes of light (photopsia): usually appear in peripheral vision, like lightning
- New floaters: a sudden increase in dark spots, cobwebs, or threads drifting across vision
- Curtain shadow: a dark veil creeping across part of your visual field from one direction
If you experience all three at once, treat it as a retinal emergency and seek care within hours.
Sudden Blind Spots or Complete Darkness
A sudden scotoma (blind spot) or total blackout in one eye, even if it lasts only a few seconds, is a serious warning sign.
Transient monocular vision loss, known as amaurosis fugax, can be a precursor to a full retinal artery occlusion or stroke and requires same-day emergency evaluation.
Vision Loss with Headache or Nausea
When sudden vision loss is accompanied by a severe headache, nausea, or vomiting, the possibilities include:
- Acute angle-closure glaucoma
- Giant cell arteritis (temporal arteritis) is common in adults over 50
- Stroke or TIA (transient ischemic attack) affecting the visual cortex
- Severe hypertensive crisis
Any combination of vision loss and neurological symptoms warrants an ER visit without delay.
Worried about screen time? Check out Blue Light Glasses Do They Really Protect Your Eyes to separate myths from facts.
Is Sudden Vision Loss Linked to Stroke?
Yes, and this connection is one of the most critical things to understand about sudden vision loss. The eyes are directly connected to the brain through the optic nerve and visual pathways.
A stroke affecting the visual areas of the brain can cause sudden vision loss as a primary or secondary symptom.
Eye Symptoms Related to Stroke
The FAST acronym (Face, Arms, Speech, Time) used for stroke awareness does not always capture vision symptoms. Eye-related stroke signs include:
- Sudden loss of vision in one eye (monocular)
- Loss of the same half of the visual field in both eyes (hemianopia)
- Double vision or inability to move the eyes together
- Drooping eyelid accompanied by pupil changes
Any of these symptoms alongside weakness, speech problems, or facial drooping should trigger an immediate emergency call.
When Brain Imaging Becomes Necessary
If sudden vision loss cannot be fully explained by an eye examination alone, or if neurological symptoms accompany it, brain imaging becomes essential. An MRI or CT scan of the brain may be ordered to:
- Rule out ischemic stroke or hemorrhagic stroke
- Detect tumors or lesions pressing on the optic pathway
- Identify demyelinating lesions associated with MS
- Evaluate for posterior cortex ischemia
How Sudden Vision Loss Is Diagnosed
Rapid and accurate diagnosis is the foundation of effective treatment. A combination of clinical examination and imaging tools is typically used in emergency settings to identify the cause.
Eye Examination Tests
An ophthalmologist will begin with a series of clinical tests to assess the eye’s structure and function:
- Visual acuity test: Checks how sharp vision is in each eye
- Slit-lamp examination: Evaluates the front part of the eye for inflammation or structural abnormality
- Dilated fundus exam: Allows direct visualization of the retina, optic disc, and blood vessels
- Intraocular pressure (IOP) measurement: Essential for detecting glaucoma
- Visual field testing: Maps the full extent of what each eye can see
Retinal Imaging and OCT Scan
Modern imaging has transformed the speed and precision of eye emergency diagnosis.
- Fundus photography: Captures a wide-field image of the retina to detect detachments, hemorrhages, and occlusions
- Optical Coherence Tomography (OCT): Provides cross-sectional retinal imaging at the cellular level, invaluable for detecting macular conditions and retinal swelling
- Fluorescein angiography (FA): Dye-based imaging to map blood flow through retinal vessels
- Ocular ultrasound (B-scan): Used when the view of the retina is blocked, such as in vitreous hemorrhage
Emergency Treatments for Sudden Vision Loss
Treatment depends on the underlying cause and how quickly the patient presents. The earlier treatment begins, the better the visual outcome. Here are the main emergency interventions used.
Laser Treatment
Laser photocoagulation is a cornerstone treatment for several retinal emergencies.
- Retinal tears: Laser is applied around the tear to create scar tissue that seals it before full detachment occurs
- Diabetic vitreous hemorrhage: Panretinal photocoagulation (PRP) destroys abnormal blood vessels
- Retinal vein occlusion: Macular laser reduces fluid leakage in certain subtypes
Eye Injections
Intravitreal injections, delivered directly into the vitreous cavity, are a major treatment advance for vision-threatening conditions.
- Anti-VEGF injections (e.g., Ranibizumab, Bevacizumab, Aflibercept): Reduce abnormal vessel growth and fluid leakage in vein occlusion, wet macular degeneration, and diabetic retinopathy
- Steroid implants or injections: Manage intraocular inflammation in conditions like uveitis and vein occlusion
Surgery for Retinal Conditions
In cases of retinal detachment or large vitreous hemorrhage, surgery is required:
- Vitrectomy: Removal of the vitreous gel, often combined with retinal repair
- Scleral buckle: A silicone band placed around the eye to push the wall against the detached retina
- Pneumatic retinopexy: A gas bubble is injected into the eye to push the retina back into place, used for certain types of detachment
Think lazy eye is only in childhood? Discover Lazy Eye Amblyopia Treatment for Adults and learn about modern treatment options.
Can Vision Return After Sudden Loss?
Recovery from sudden vision loss depends heavily on the cause, the severity, and, most critically, how quickly treatment is started. Outcomes range from complete recovery to permanent impairment.
Cases with Full Recovery
Several conditions can result in full or near-full visual recovery with timely treatment:
- Retinal tear (treated before detachment): Excellent prognosis with laser or cryotherapy
- Vitreous hemorrhage (without retinal damage): Vision often clears as the blood absorbs over weeks
- Optic neuritis: Most patients regain good vision within weeks to months
- Acute angle-closure glaucoma (treated within hours): Pressure can be lowered, preserving vision
Conditions That May Cause Permanent Damage
Some causes of sudden vision loss carry a high risk of permanent impairment, particularly without prompt treatment:
- Central retinal artery occlusion: Permanent damage can occur within 90-100 minutes of onset
- Macula-involving retinal detachment: Central vision may not fully recover even after surgery
- Giant cell arteritis: Irreversible blindness can occur if not treated with urgent steroids
- Advanced glaucoma: Optic nerve damage is irreversible once it occurs
Who Is at Higher Risk of Sudden Vision Loss?
Certain health conditions and demographic factors significantly raise the risk of experiencing sudden vision loss. Understanding your personal risk can motivate proactive eye care.
Diabetes and Blood Pressure Patients
Patients with poorly controlled diabetes or hypertension face a substantially elevated risk due to the damage these conditions inflict on small blood vessels throughout the body, including those in the retina.
- Diabetic retinopathy is the leading cause of vision loss in working-age adults
- Hypertension can cause retinal vein occlusion, optic neuropathy, and hypertensive retinopathy
- Both conditions dramatically increase the risk of retinal artery occlusion
Annual dilated eye exams are strongly recommended for all diabetic patients regardless of symptoms.
Older Adults and Glaucoma Risk
Age is the single greatest risk factor for most serious eye conditions. After the age of 60, the risk of acute angle-closure glaucoma, macular degeneration, and retinal vascular disease all rise significantly.
- Individuals of East Asian and South Asian descent have a higher anatomical predisposition to angle-closure glaucoma
- Farsighted individuals (hyperopia) are at a higher structural risk of narrow angles
- A family history of glaucoma increases personal risk by 4 to 9 times
When to See an Eye Specialist Immediately
Do not wait for a routine appointment if you experience any of the following. These symptoms require the same-day or emergency ophthalmology evaluation:
- Any sudden loss of vision in one or both eyes, even if temporary
- A new curtain, shadow, or veil across part of your visual field
- A sudden shower of new floaters, especially with flashes of light
- Severe eye pain with reduced vision, headache, or nausea
- Double vision appearing without a prior diagnosis
- Vision loss accompanied by facial drooping, arm weakness, or speech difficulty
When in doubt, go to the emergency room. There is no such thing as being too cautious with sudden vision changes.
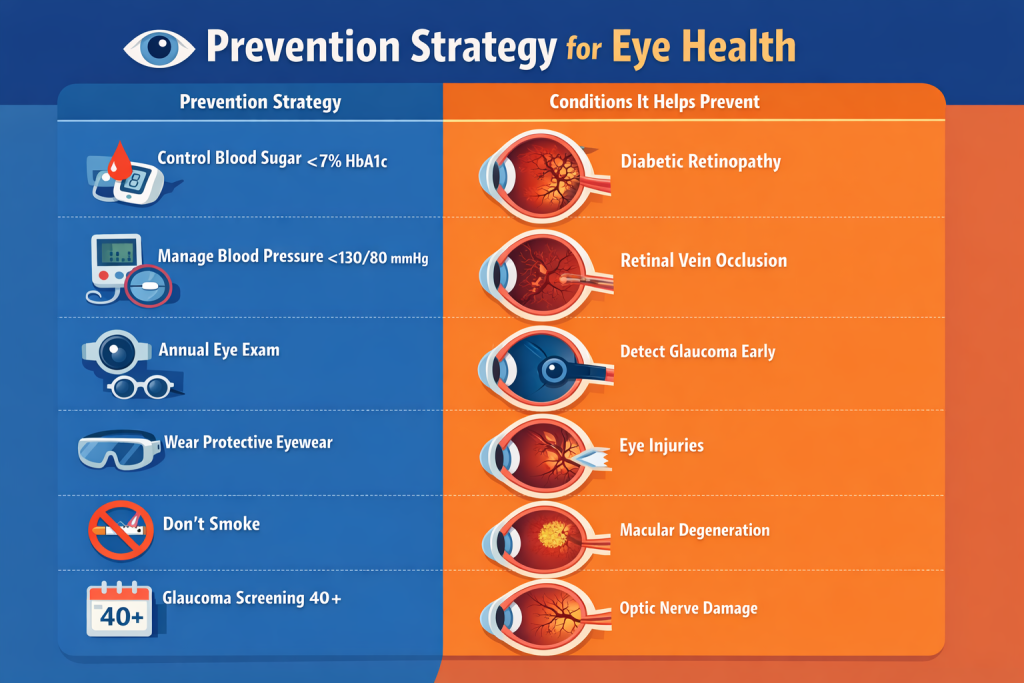
Preventing Serious Eye Emergencies
While not all causes of sudden vision loss can be prevented, many risk factors are modifiable. Here are the most impactful prevention strategies:
Struggling to see clearly at night? Explore Night Vision Problems Causes Symptoms and Treatment to understand what your eyes might be telling you.
Conclusion
Sudden vision loss is never something to sleep off or monitor for a few days. Whether it is painless or painful, total or partial, transient or persistent, it is a medical emergency that demands immediate evaluation. The window for effective treatment in many conditions is measured in minutes to hours, not days.
From retinal detachment and eye stroke to glaucoma and optic neuritis, the conditions that cause sudden vision loss are serious, but many are treatable when caught in time. Know your risk factors, attend regular eye check-ups at Seedieye Care Centre, Bangalore, and most importantly, act immediately if something suddenly changes in your vision. Your eyesight is irreplaceable.
Frequently Asked Questions
1. Can sudden vision loss go away on its own?
Transient vision loss may resolve within minutes, but this does not mean the underlying cause is harmless. A temporary episode of vision loss, especially in one eye, is often a warning sign of an impending stroke or retinal artery occlusion.
2. How quickly does sudden vision loss need to be treated?
For conditions like central retinal artery occlusion, the treatment window can be as short as 90 minutes, similar to a brain stroke. Retinal detachment involving the macula also demands same-day surgery for the best outcomes.
3. Is sudden vision loss in one eye more serious than in both?
Both are serious, but they point to different causes. Vision loss in one eye usually suggests a problem in the eye itself, such as retinal detachment or artery occlusion.
4. What is the most common cause of sudden vision loss in diabetic patients?
In diabetic patients, the most common cause of sudden vision loss is vitreous hemorrhage, bleeding into the eye from fragile, abnormal blood vessels that develop due to diabetic retinopathy.
5. Can stress or anxiety cause sudden vision loss?
While extreme psychological stress can occasionally trigger vasospasm, which may briefly affect vision, this is rare and should still be medically evaluated. Stress alone is generally not a direct cause of sudden vision loss.